People with chronic fatigue syndrome have often complained they are not taken seriously but that could change as research is done into similar effects from the coronavirus
By Sean O'Neill, 19 August 2021
Extracts
Stacey [Fresco] was one of the first people in the country to attend a long Covid clinic but has since been discharged… “My sister puts it very well. She says ‘Stacey looks really well on the outside but on the inside, not so great’. To be honest, it’s exhausting and it’s exhausting to feel this bad all the time.”
Stacey’s family has experience of chronic illness and if the doctors who saw her last year didn’t know what was wrong with her, she has a pretty clear idea. Her long Covid, she says, “correlates strongly with ME, the similarities are striking”.
Her recognition, as a patient, of the overlap between long Covid and myalgic encephalomyelitis (ME), also sometimes called chronic fatigue syndrome (CFS), is increasingly shared by the scientific community.
Anthony Fauci, the man heading the United States response to the pandemic, sparked debate when he talked of the issue a year ago just as long Covid was coming to be recognised as a major problem.
“It’s extraordinary how many people have a post-viral syndrome that’s very strikingly similar to myalgic encephalomyelitis/chronic fatigue syndrome,” he told Medscape. “They just don’t get back to normal energy or normal feeling of good health.”
Eleanor Riley, professor of immunology at Edinburgh University, wrote in The Scotsman last month that “an ME/CFS-like syndrome is emerging as a long-term consequence of Covid-19”.
Misunderstood, misdiagnosed
In new research from the US, Anthony Komaroff from Harvard medical school and Ian Lipkin of Columbia University suggest long Covid and ME have the same origin and development.
“The Covid-19 pandemic is likely to greatly increase the number of people who develop ME/CFS or a similar illness and other post-Covid illnesses,” they wrote. “It seems likely that the underlying biology [of long Covid] is similar to that of other post-infectious fatigue syndromes, to post-critical illness syndrome, and to that of ME/CFS.”
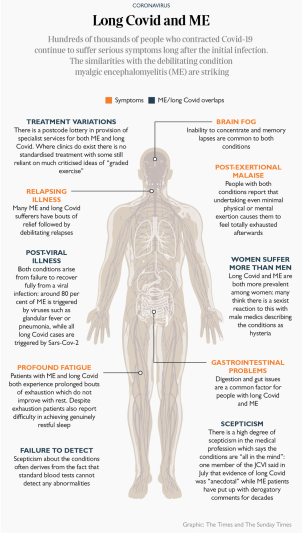
ME is a debilitating condition, usually triggered by a viral infection, in which the body seems to turn on itself causing multiple symptoms including brain fog, profound fatigue, limb and muscle pain, gastrointestinal difficulties and dizziness. It is often (but not always) a relapsing illness, characterised by crashes and flare-ups particularly if the sufferer exerts themselves even a fraction too much. Some patients become severely ill and are confined to their homes or beds.
For years a core treatment recommended by the NHS and the National Institute for Health and Care Excellence (NICE) was “graded exercise therapy”.
The ME patient community has complained for years that tens of thousands of people have been advised to undertake exercise regimes which caused relapse rather than rehabilitation. The Centre for Disease Control in the United States has for some time advised against such exercise programmes, warning patients cannot tolerate them and saying “exercise cannot be expected to be a cure”.
Nice was supposed to remove graded exercise as a treatment in new guidelines earlier this week, but delayed their publication under pressure from leading medical bodies, including the Royal College of Physicians, which believe the therapy is still useful. It was a decision that sparked further controversy in the bitter debate over ME that has raged for decades…
The symptoms that have made life so hard for ME sufferers — of whom there are an estimated 250,000 in the UK — are now being examined more closely because they are being repeated in people with long Covid. Surveys by the Office for National Statistics have found 385,000 people in the UK suffering the after-effects of Covid-19 more than a year after their initial infection. Many are being diagnosed with ME and turning to ME charities for help.
The government boasts of opening dozens of long Covid clinics across the country but provision is patchy, treatment varied — with many offering the kind of exercise regimes that ME patients have complained of — and the efficacy questionable.
The experiences of long Covid patients often mirror those of people with ME who complain of inadequate and ineffective treatment in the places where it can be found…

Research
Dr David Strain, of the University of Exeter, encountered long Covid early in the pandemic in patients with ME and initially thought the coronavirus was another trigger for relapses in their conditions…
Strain is also part of a consortium recently awarded £6 million of public funding to study potential treatments. Some of the medications he will trial have been used with some success to alleviate symptoms of ME patients.
“I’m a scientist so obviously I will never say anything for certain until I get some sort of concrete evidence, but I am working on the assumption that these are very similar conditions,” he said.
“The silver lining to this cloud is that all the money that’s going into looking for the underlying causes of long Covid is mirroring what’s already known about ME/CFS. For example, we know long Covid is more common in females and people who are atopic — people who have asthma, eczema, those sorts of conditions — which is in keeping with it being a hyperactive immune response, and that’s something that’s previously been seen with CFS/ME.”
Strain is also leading a study searching for the genetic markers of long Covid which will co-operate with the Decode ME project set to begin collecting DNA samples from ME patients next month. Researchers will be comparing the results of the studies.
Strain says: “The learning we get from long Covid can also be implemented in the ME world.”
The research drive is long overdue. ME has attracted little public funding in the UK while conditions such as cancer and Alzheimer’s have benefitted from vast amounts of public and charity cash. The realisation that long Covid poses a major health challenge is starting to change that picture and the National Institute of Health Research announced a £20 million fund in July. In the US the issue is being taken even more seriously and the National Institutes of Health is pumping $1.1 billion into a programme of research projects…